Whereas last week we talked about the association between psychotic disorders and moving to a different country (which you can read about here), another one of our recent papers, published in last month’s issue of JAMA Psychiatry, found that, before age 20, the greater the distance moved within a country, the greater the risk to be diagnosed with a non-affective psychotic disorder (such as schizophrenia).
 It is not uncommon to move house during childhood and adolescence, for example due to financial problems or a change of parental employment in the household. These time periods are important for social development and may be a central stressor when migrating is the breaking up of social networks. Moving during childhood may be associated with changing schools, meaning young people could be faced with the challenges of fitting in with a new peer group. Social isolation and lack of peer relationships have been previously found to be associated with psychotic disorders (Winsper, Wolke, Bryson, Thompson, & Singh, 2016), and consistent with this, research has also found a link between psychotic disorders and moving houses during childhood and adolescence (Paksarian, Eaton, Mortensen, & Pedersen, 2015).
It is not uncommon to move house during childhood and adolescence, for example due to financial problems or a change of parental employment in the household. These time periods are important for social development and may be a central stressor when migrating is the breaking up of social networks. Moving during childhood may be associated with changing schools, meaning young people could be faced with the challenges of fitting in with a new peer group. Social isolation and lack of peer relationships have been previously found to be associated with psychotic disorders (Winsper, Wolke, Bryson, Thompson, & Singh, 2016), and consistent with this, research has also found a link between psychotic disorders and moving houses during childhood and adolescence (Paksarian, Eaton, Mortensen, & Pedersen, 2015).
Until now, it has remained unclear whether this impact extended beyond mid-adolescence, and into moves in late adolescence and adulthood. We hypothesized that there would be a positive relationship between amount of times moved during childhood and adolescence and later risk of non-affective psychotic disorders. Additionally, we predicted that the greater the distance moved, the greater this risk would be, being strongest when distances moved were most likely to indicate a breakup of social networks (we set this to be 30 km, a distance we hypothesised would likely involve changing schools) .
Our study included 1.4 million participants, all Swedish residents born between 1982 and 1995. They were followed from birth to age 29. We were interested in four time periods: early childhood (0-6 years), childhood (7-15 years), adolescence (16-19 years) and early adulthood (20-29 years). Data on non-affective psychotic diagnoses were collected, as well as additional information such as sex, family income, educational attainment, and parental history of mental illness from the Swedish registers.
As predicted, residential mobility was associated with non-affective psychosis. For all time periods, a change in residence significantly increased the risk, often by number of times moved. For example; moving once over the time period of 16-19 years old increased the risk with 28% but moving four times or more doubled the risk. The pattern was different in early adulthood, where increased risk was notable only when the amount of times moved was 3 or more. Also consistent with our predictions, greater distance moved led to greater risk. However, this was only true during childhood and adolescence, as early adulthood yielded a decrease in risk compared to the general Swedish population (see graph).
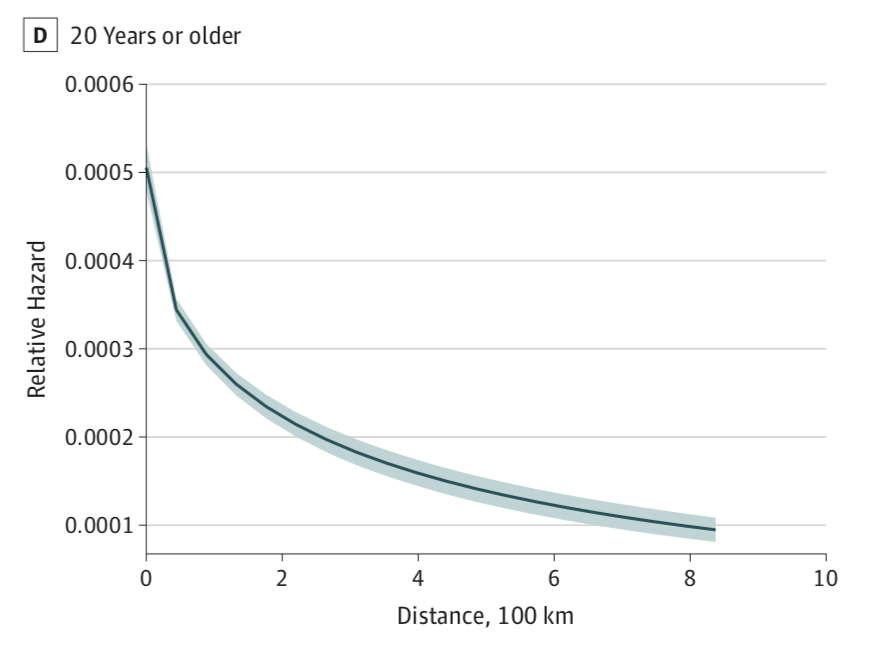
During childhood and adolescence, a change in residence is likely initiated by guardians. Our results could be explained in that the breakup of social networks when moving disrupts the developing ability to make new friends and maintain friendships. This could lead to increased social isolation, which again makes one vulnerable to mental illness including psychotic disorders. However, past 20 years old, moving is likely a personal choice by the individual. We found that longer distances moved predicted a lower likelihood of being diagnosed with a non-affective psychotic disorder past 20 years old. This could be explained by the fact that the personal choice made reflects health and independence as the individual moves out from their parent’s house and enters work or attends university. Meanwhile, it would be more difficult for individuals vulnerable to non-affective psychotic disorders to move out and enter work or university, due to symptoms revolved around cognitive deficits as well as the strong association between psychotic disorders and social defeat (Dickson, Laurens, Cullen, & Hodgins, 2012; Selten, van der Ven, Rutten, & Cantor-Graae, 2013).
Our paper published last week found that for all ages investigated, including childhood, adolescence and early adulthood, migrating to a different country increased the risk of being diagnosed with a psychotic disorder. This paper, as well as the one on moving houses within a country, support the idea that migration involving disruption of social networks appear to increase risk, especially for international migrants. This might be particularly difficult for visible minorities. Greater differences, both visible and not, involves greater difficulty for a child to fit in with a peer group. A good network of social support, including both family and peer-relationships, is crucial as a preventive measure against psychotic disorders. Hence, it is important that children and adolescents receive the necessary attention and support when migrating, both internationally and within a country, to minimize risks of a future diagnosis.
References:
Paksarian, D., Eaton, W. W., Mortensen, P. B., & Pedersen, C. B. (2015). Childhood residential mobility, schizophrenia, and bipolar disorder: a population-based study in Denmark. Schizophr Bull, 41(2), 346-254.
Selten, J. P.,van der Ven, E., Rutten, B. P. F., & Cantor-Graae E. (2013). The social defeat hypothesis of schizophrenia: an update. Schizophr Bull, 39 (6), 1180-1186.
Winsper, C., Wolke, D., Bryson, A., Thompson, A., & Singh, S. P. (2016). School mobility during childhood predicts psychotic symptoms in late adolescence. J Child Psychol Psychiatry, 57 (8), 957-966.
Dickson, H., Laurens, K. R., Cullen, A. E., & Hodgins, S. (2012). Meta-analyses of cognitive and motor function in youth aged 16 years and younger who subsequently develop schizophrenia. Psychol Med, 42(4), 743-755.